Identifying Pain Triggers: How Data Reveals What Memory Cannot
I’m the developer behind CrisisCore-Systems and Pain Tracker – a privacy-first, offline-first pain journal built for people who’ve been failed by “normal” health apps. I build PWAs that run entirely on your device, use real encryption, and respect trauma and crisis instead of exploiting them. Here I write about Web Crypto, IndexedDB, workers’ comp evidence, and building software from collapse.
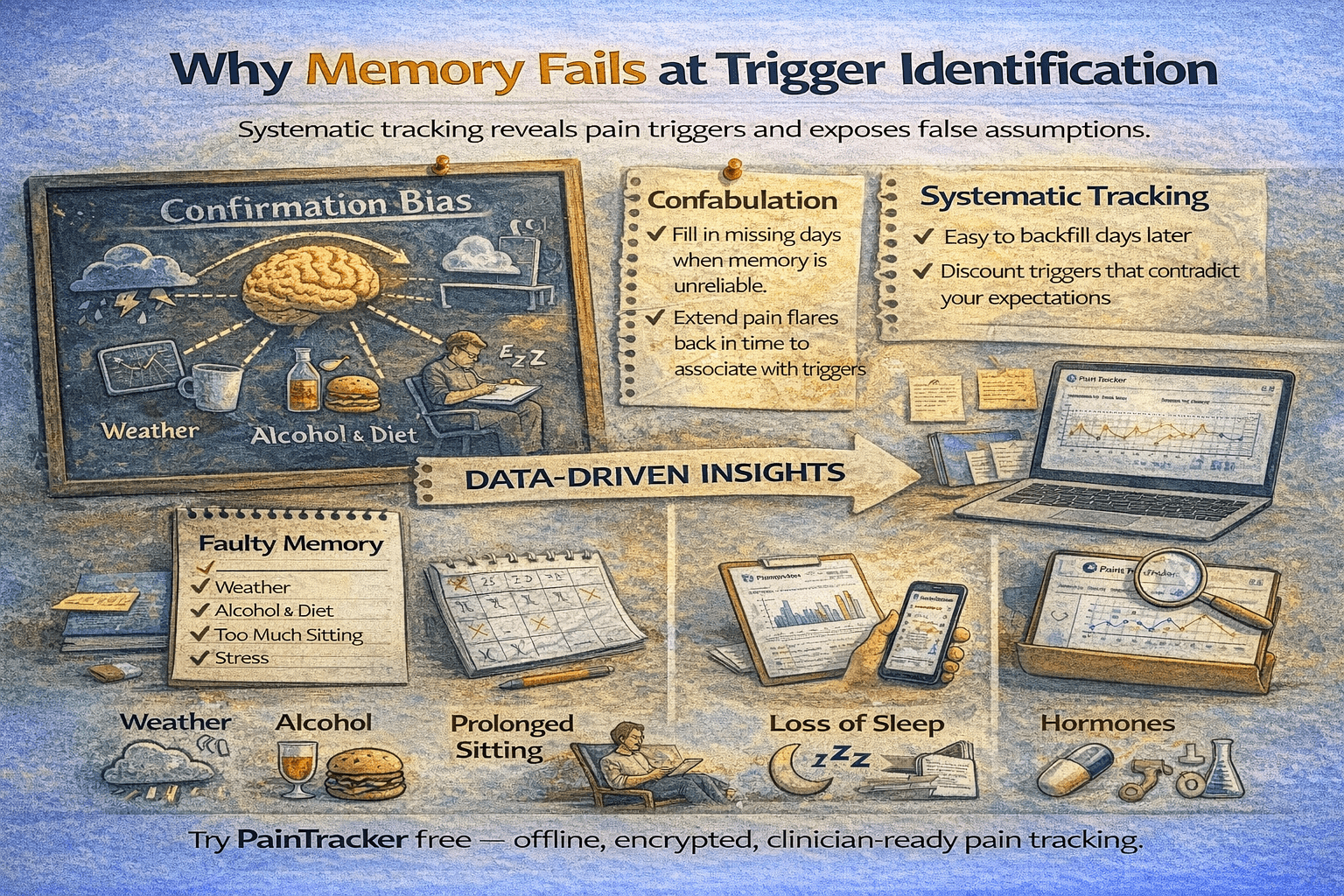
Why memory fails at trigger identification
Human memory is poorly suited to identifying correlations across multiple variables over time. When you experience a pain flare, you naturally look for an immediate cause—but many triggers operate with a delay of hours or days. Weather changes may precede flares by 24 hours. Sleep disruption may not affect pain levels until the second night. Stress accumulates before manifesting physically. These delayed relationships are nearly invisible to retrospective recall.
Confirmation bias compounds the problem. Once you believe something is a trigger, you notice it before every flare and overlook the times it occurred without consequences. Structured tracking bypasses both limitations by recording potential triggers consistently, regardless of whether a flare follows, creating a dataset that reveals genuine correlations while filtering out coincidences.
Common pain triggers worth tracking
The most frequently identified pain triggers across chronic pain conditions include: physical overexertion, prolonged static postures (sitting, standing), sleep disruption or insufficient sleep, emotional stress, weather changes (barometric pressure drops, temperature shifts, humidity), dietary factors (alcohol, specific foods), hormonal fluctuations, and illness or infection.
PainTracker lets you record these potential triggers through tags, structured fields, and notes alongside your daily pain entries. The key is consistency: record the same trigger categories every day, not just on days when you think they might be relevant. This creates the complete dataset needed for meaningful correlation analysis.
Systematic trigger investigation
Rather than tracking everything simultaneously, investigate triggers systematically. Start with two or three candidate triggers based on your clinical suspicion and track them consistently for four to six weeks. Then review the data: do high-pain days consistently follow days with the suspected trigger? Is the relationship statistically meaningful or just occasional?
PainTracker's local analytics can help visualise these correlations on your device. Weather data integration shows barometric pressure alongside your pain entries. Time-of-day analysis reveals whether morning, afternoon, or evening pain dominates. Activity-pain correlation views show whether busy days predict worse pain the next day.
Weather as a pain trigger
The relationship between weather and pain is widely reported by patients but inconsistently supported by population-level research—likely because the relationship varies significantly between individuals. Some people are sensitive to barometric pressure changes, others to temperature, and many to combinations that are unique to their condition.
PainTracker integrates local weather data to automatically correlate your pain entries with barometric pressure, temperature, and humidity. This person-specific analysis can confirm or rule out weather sensitivity for you individually—a much more useful result than population-level studies that average across different sensitivities.
Using trigger data for proactive management
Identified triggers are actionable. If prolonged sitting consistently precedes higher pain, you can schedule movement breaks. If barometric pressure drops predict flares, you can pre-medicate or adjust your schedule on forecast-change days. If poor sleep reliably increases next-day pain, sleep hygiene becomes a concrete pain management intervention rather than generic lifestyle advice.
Share your trigger findings with your care team. A clinician who knows that your flares follow a specific pattern can tailor treatment recommendations, suggest targeted interventions, and help you develop a proactive management plan based on your personal trigger profile rather than generic guidelines.
Try PainTracker free — offline, encrypted, clinician-ready pain tracking.